Rash, Lymphadenopathy, and Nephritis: Is It Always Lupus?
DOI:
https://doi.org/10.59652/2v2egm39Keywords:
IgG4-related disease, tubulointerstitial nephritis, hypocomplementemia, lymphadenopathy, vasculitisAbstract
Background: IgG4-related disease (IgG4-RD) is a multisystem fibroinflammatory condition capable of affecting nearly any organ. Renal involvement, although recognized, remains uncommon and frequently leads to diagnostic uncertainty because of overlap with autoimmune, infectious, and lymphoproliferative disorders.
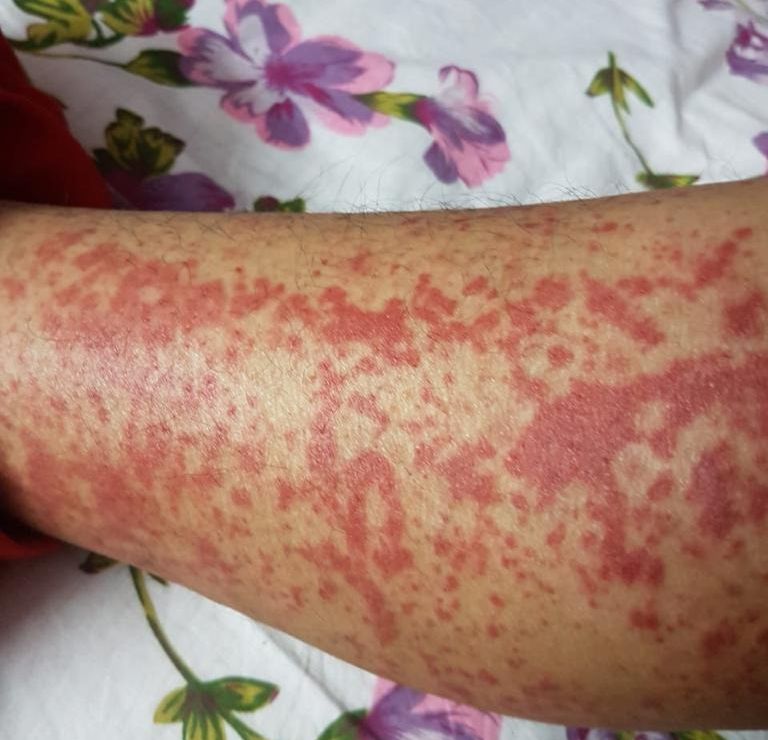
Case Presentation: A 34-year-old woman presented with a three-year course of intermittent painful purpuric plaques, chronic cough, Raynaud-like digital pallor, and episodic arthralgia. Examination revealed generalized non-tender lymphadenopathy. Laboratory studies showed anemia, eosinophilia, low complement levels, elevated IgG, and renal dysfunction. Autoimmune markers were negative. Imaging identified right-sided bronchiectatic changes and axillary lymphadenopathy. Skin biopsy showed leukocytoclastic vasculitis, while lymph node histology suggested reactive plasma cell-rich changes. A markedly raised serum IgG4 level (>53 g/L) prompted kidney biopsy, which demonstrated storiform fibrosis and abundant IgG4-positive plasma cells, confirming IgG4-related tubulointerstitial nephritis.
Discussion & Conclusion: The combination of renal, cutaneous, pulmonary, and lymph node abnormalities, together with serological and histopathological findings, established the diagnosis of systemic IgG4-RD and illustrated its ability to mimic a broad differential diagnosis.
Prednisolone therapy resulted in clinical and biochemical improvement, including normalization of renal function and improvement in complement levels. The patient remains in remission at 1 year.
Downloads
References
1. Stone JH, Zen Y, Deshpande V. IgG4-related disease. N Engl J Med. 2012;366(6):539-551.
2. Umehara H, Okazaki K, Masaki Y, Kawano M, Yamamoto M, Saeki T, et al. A novel clinical entity, IgG4-related disease (IgG4-RD): general concept and details. Mod Rheumatol. 2012;22(1):1-14.
3. Wallace ZS, Naden RP, Chari S, Choi HK, Della-Torre E, Dicaire JF, et al. The 2019 American College of Rheumatolo-gy/European League Against Rheumatism classification criteria for IgG4-related disease. Ann Rheum Dis. 2020;79(1):77-87.
4. Raissian Y, Nasr SH, Larsen CP, Colvin RB, Smyrk TC, Takahashi N, et al. Diagnosis of IgG4-related tubulointerstitial nephritis. J Am Soc Nephrol. 2011;22(7):1343-1352.
5. Deshpande V, Zen Y, Chan JKC, Yi EE, Sato Y, Yoshino T, et al. Consensus statement on the pathology of IgG4-related disease. Mod Pathol. 2012;25(9):1181-1192.
6. Saeki T, Nishi S, Imai N, Ito T, Yamazaki H, Kawano M, et al. Clinicopathological characteristics of patients with IgG4-related kidney disease. Kidney Int. 2010;78(10):1016-1023.
7. Inoue D, Zen Y, Abo H, Gabata T, Demachi H, Kobayashi T, et al. Immunoglobulin G4-related lung disease: CT findings with pathologic correlations. Radiology. 2009;251(1):260-270.
8. Della-Torre E, Lanzillotta M, Doglioni C. Immunology of IgG4-related disease. Clin Exp Immunol. 2015;181(2):191-206.
9. Khosroshahi A, Wallace ZS, Crowe JL, Akamizu T, Azumi A, Carruthers MN, et al. International consensus guidance statement on the management and treatment of IgG4-related disease. Arthritis Rheumatol. 2015;67(7):1688-1699.
10. Kamisawa T, Zen Y, Pillai S, Stone JH. IgG4-related disease. Lancet. 2015;385(9976):1460-1471.
Downloads
Published
Issue
Section
License
Copyright (c) 2026 Annals of Innovation in Medicine

This work is licensed under a Creative Commons Attribution 4.0 International License.





